Cardiovascular Inpatient Service
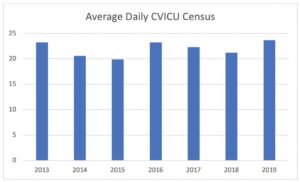 The Cardiovascular Inpatient Service at the Arkansas Children’s Hospital Heart Center consists of a 31-bed Cardiovascular Intensive Care Unit (CVICU) that is strategically located adjacent to a pair of dedicated cardiac ORs. The new cath labs are also located near the CVICU. The providers working in the CVICU are separated into an intensive care team and an intermediate team.
The Cardiovascular Inpatient Service at the Arkansas Children’s Hospital Heart Center consists of a 31-bed Cardiovascular Intensive Care Unit (CVICU) that is strategically located adjacent to a pair of dedicated cardiac ORs. The new cath labs are also located near the CVICU. The providers working in the CVICU are separated into an intensive care team and an intermediate team.
The CVICU manages patients with all forms of pediatric and congenital cardiac disease:
- Pre- and postoperative care
- Cardiac transplantation
- Medical management
- Cardiac arrhythmias
- Heart failure with all modalities of mechanical support (ECMO, all types of VADs)
At the foundation of the Heart Center’s CVICU is our multi-disciplinary team model. Cardiologists and cardiac intensivists work collaboratively with surgeons, nurse practitioners, medical students, nurses, respiratory therapists, dieticians, occupational therapists, physical therapists, and case managers. Each member of the team is integral to providing comprehensive care to our patients and their families. On a given day, two dedicated teams provide clinical care:
- The Intensive Care Team includes an attending physician, 1-2 fellows (cardiology, pediatric ICU, neonatal ICU, and CV anesthesia), and advanced nurse practitioners. There is 24/7 in-house coverage in the CVICU by an attending cardiac intensivist.
- The Intermediate Team includes an attending cardiologist and advanced nurse practitioners, as well as cardiology fellows intermittently. This team manages the transition from intensive care to discharge readiness, in addition to moderate acuity hospitalization of cardiac patients.
Residents and medical students are able to participate in elective rotations with either inpatient team.

Quality and safety are high priorities for the inpatient service. We support an extremely robust Quality and Safety improvement process internally. Furthermore, both the inpatient services are benchmarked to national standards with our peers in the country through our active participation in the Pediatric Cardiac Critical Care Consortium (PC4) and Pediatric Acute Care Cardiology Collaborative (PAC3).
The inpatient service faculty provide an enriching learning experience for all learners with bedside teaching, didactics, and case-based lectures. The CVICU also provides advanced training opportunities through two CVICU fellowship-training positions offered annually.
Categorical cardiology fellows are an integral part of both the CVICU and intermediate teams. The expectations and roles of the cardiology fellows typically start with first-year fellows serving as the primary provider for a group of patients and progress to third-year fellows running rounds and managing the entire team.
Consultative Cardiology
For our categorical pediatric cardiology fellows, the cardiology consult service is their primary opportunity to develop their skills as a consulting subspecialist. As the only pediatric cardiology group in the state, consult questions come from throughout our region, including within our own hospital walls and as far as our neighboring states. The wide scope of questions is both the greatest challenge and the greatest strength of this core rotation. Fellows develop an increasing degree of autonomy as they progress throughout their training, but always have the backup and supervision of an attending cardiologist.
- The consult fellow and attending are charged with interpretation of all in-house electrocardiograms ordered by non-cardiologists, as well as any outside electrocardiograms sent for formal reading, so proficiency in pediatric ECG interpretation is gained quickly.
- The consult team also evaluates urgent outpatients, such as a neonate with a worrisome heart murmur, who might otherwise be poorly served waiting for the next available clinic visit.
- Consult calls frequently come from other inpatient units, including Arkansas Children’s 104-bed level 4 Neonatal Intensive Care Unit, our 26-bed Pediatric Intensive Care Unit, and our level 1 trauma center Emergency Department.
 A typical day for the consult fellow might include evaluating a “new blue” cyanotic newborn in the NICU, examining and counseling several outpatients whose cardiac evaluations were deemed urgent, answering a handful of referring pediatrician calls about cardiology patients with possibly concerning new symptoms and cardioverting a 28-year-old in the ED with palliated complex single ventricle heart disease and recurrent atrial dysrhythmias. The consult service is the rotation where the fellow gets to meld together his/her experience from all other sub-subspecialty rotations, to help pediatricians and other specialists formulate a thoughtful cardiac plan of care.
A typical day for the consult fellow might include evaluating a “new blue” cyanotic newborn in the NICU, examining and counseling several outpatients whose cardiac evaluations were deemed urgent, answering a handful of referring pediatrician calls about cardiology patients with possibly concerning new symptoms and cardioverting a 28-year-old in the ED with palliated complex single ventricle heart disease and recurrent atrial dysrhythmias. The consult service is the rotation where the fellow gets to meld together his/her experience from all other sub-subspecialty rotations, to help pediatricians and other specialists formulate a thoughtful cardiac plan of care.