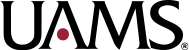Background
Of all forms of facial clefts, the Tessier No. 3 (oro-nasal-ocular clefts) is the rarest and most challenging. In 2018, pediatric otolaryngologist and cleft specialist Larry D. Hartzell, M.D., and a team of surgeons at Arkansas Children’s Hospital/UAMS treated two patients with Tessier No. 3 clefts within months of each other.
Both were born at 38 weeks gestation and had multiple associated anomalies. While both patients had a bilateral cleft lip and palate, Patient 1 had a severe left-sided cleft and Patient 2 had a right-sided incomplete cleft. The multidisciplinary team included plastic surgeon Michael S. Golinko, M.D., now at Vanderbilt Children’s Hospital, and UAMS ophthalmologist John D. Pemberton, D.O.
The basic surgical sequence for both infants was a dorsal nasal Reiger flap to level the ala, cheek advancement flap along with medial canthal repositioning, and more traditional bilateral cleft lip repair using a modified Millard technique.
Both infants are still followed for routine cleft clinical and surgical care and evaluations such as annual 3-dimensional computed tomography scans to evaluate the soft tissue and bony growth.
Patient 1
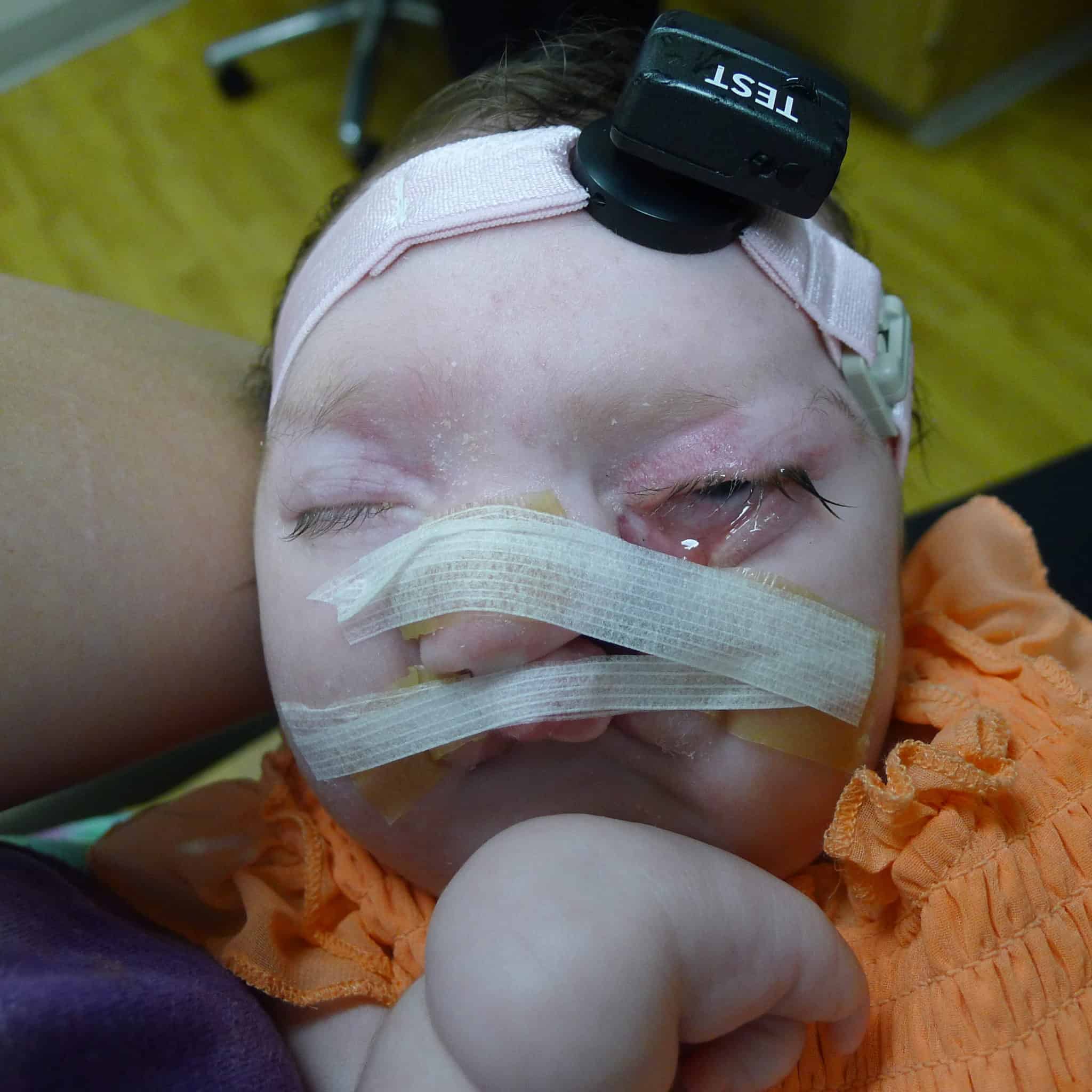
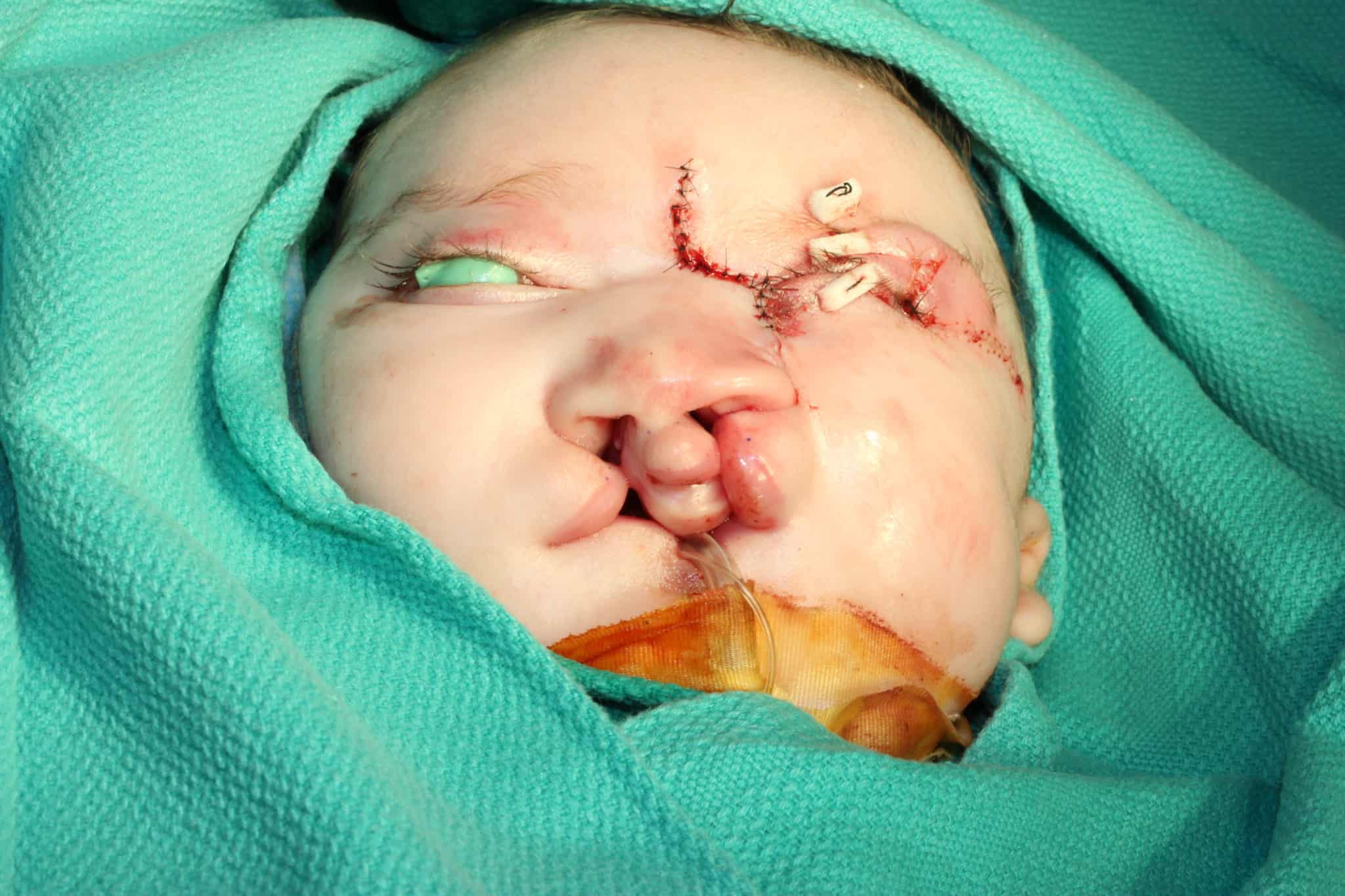
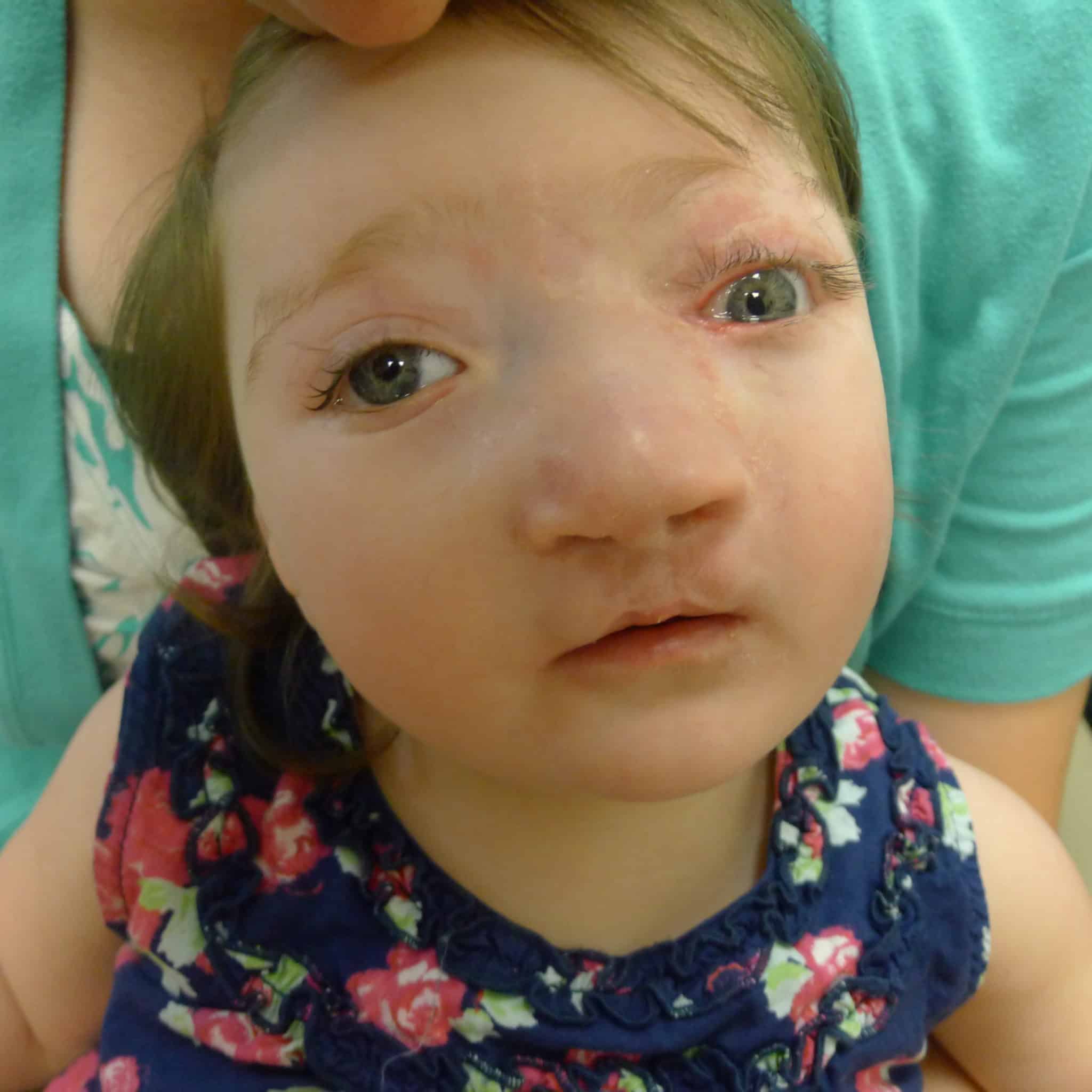
The team began consulting on the case before birth because ultrasound imaging revealed the cleft lip. The patient also had a large hole in her skull through which brain matter was extruding, and it was clear she had several other anomalies. Examination after birth revealed the child had bilateral cleft lip and palate as well as a left-sided facial cleft. She was blind in her right eye and profoundly deaf.
The oculoplastic examination revealed details of the cleft as well as parts of the face that were shortened, displaced or rotated. For example, the upper lip was rotated about 45 degrees. Parts of the nose where it attaches to the lower face were rotated and near the eye. Her lower left eyelid was shortened.
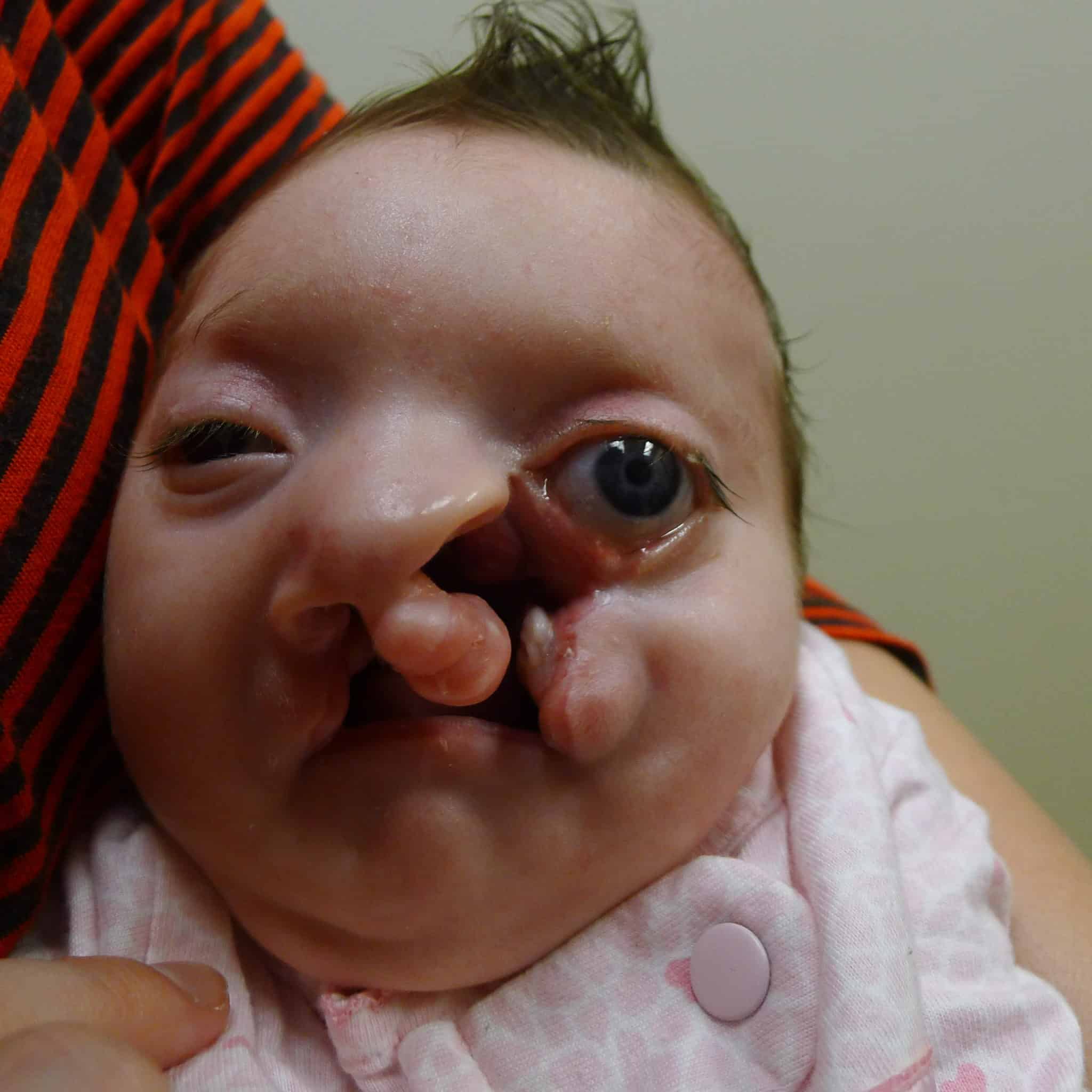
As the patient underwent other surgeries to address the hole in her skull and other issues, the craniofacial team discussed best next steps. Main goals were to rotate parts of the nose down toward the upper lip, close the lip, close the eyelid and align structures like the eye and nose. The team opted to work in stages, using taping first at 2 months of age to better position tissues and bone for upcoming surgery.
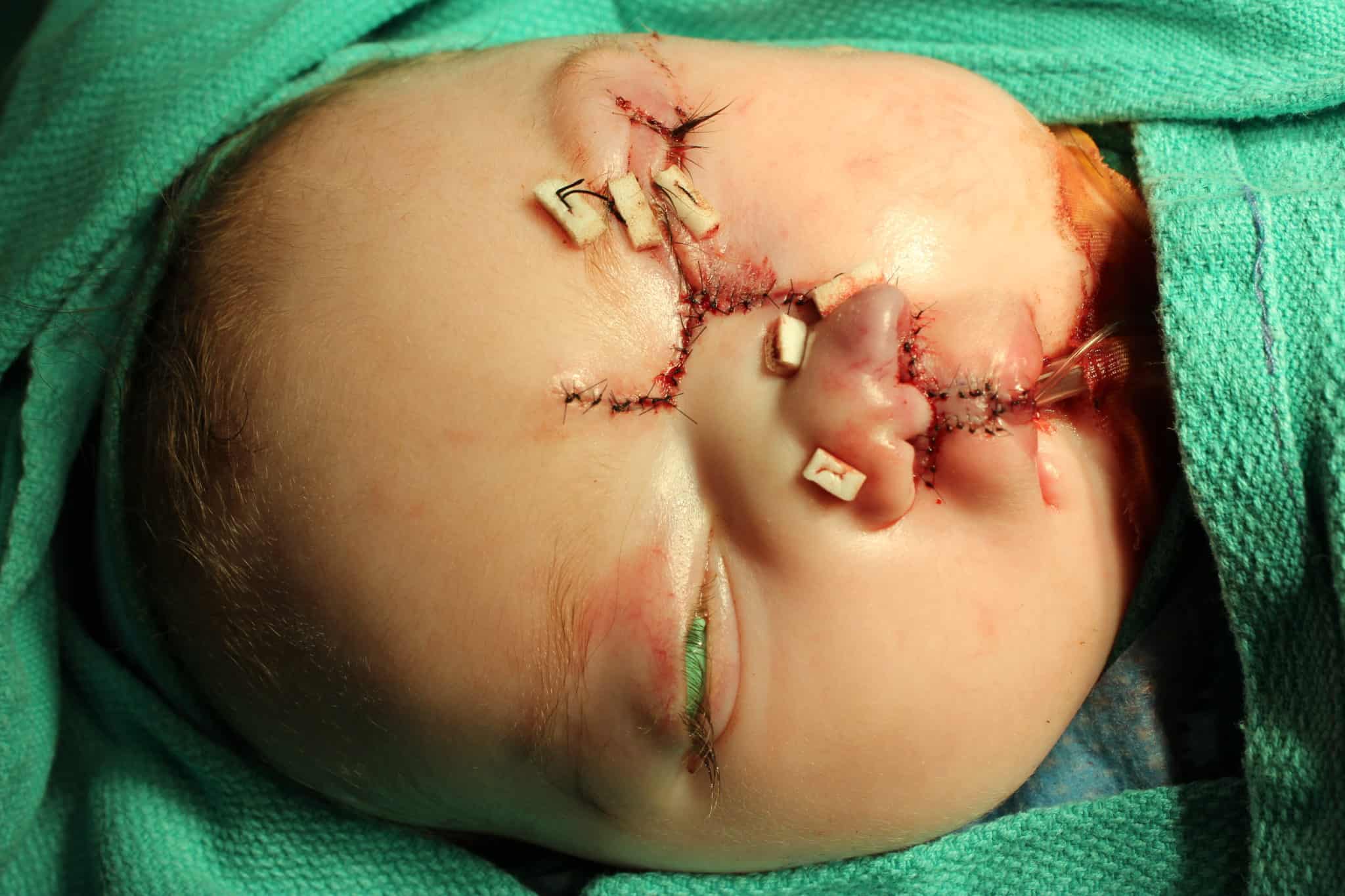
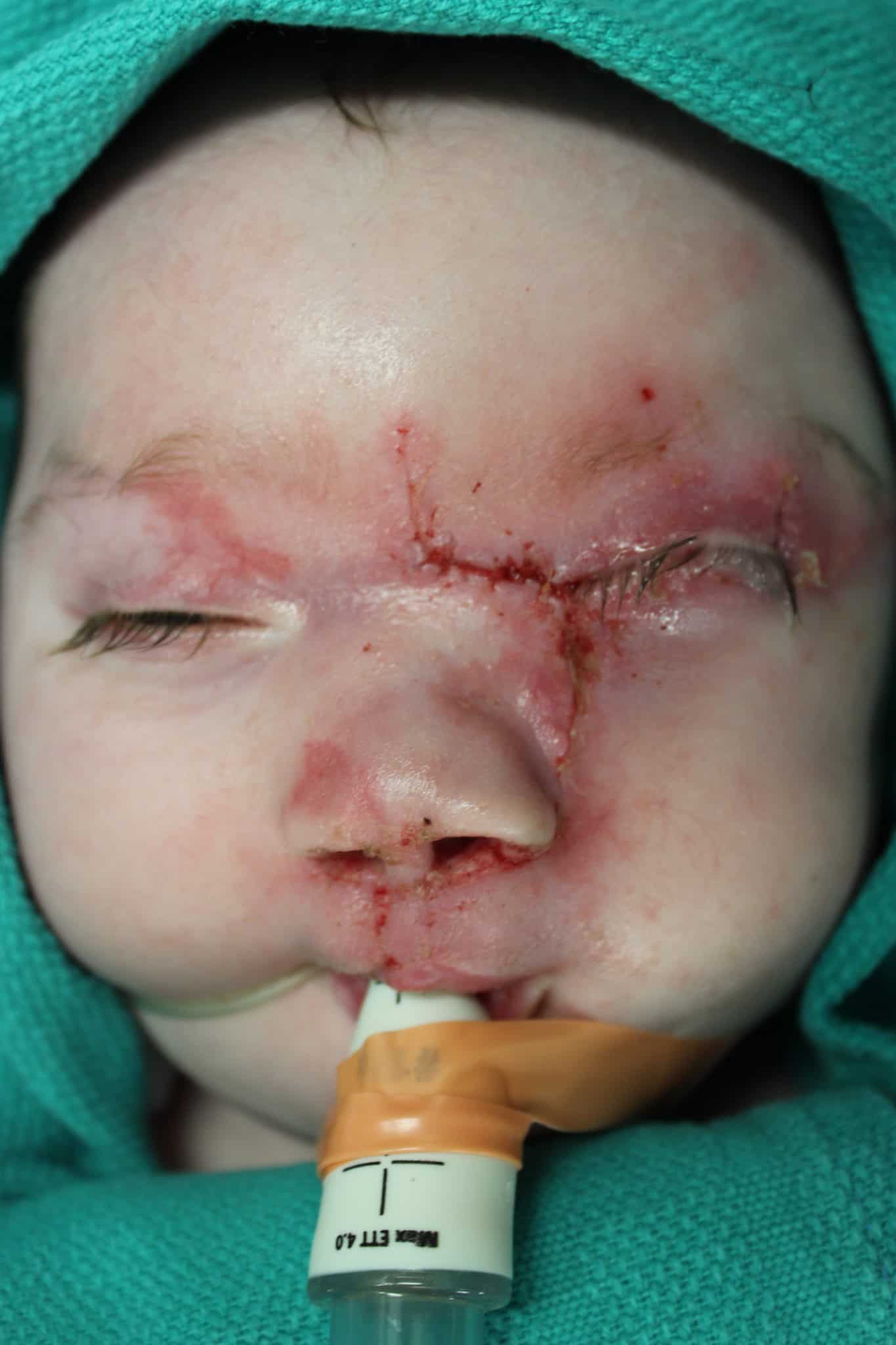
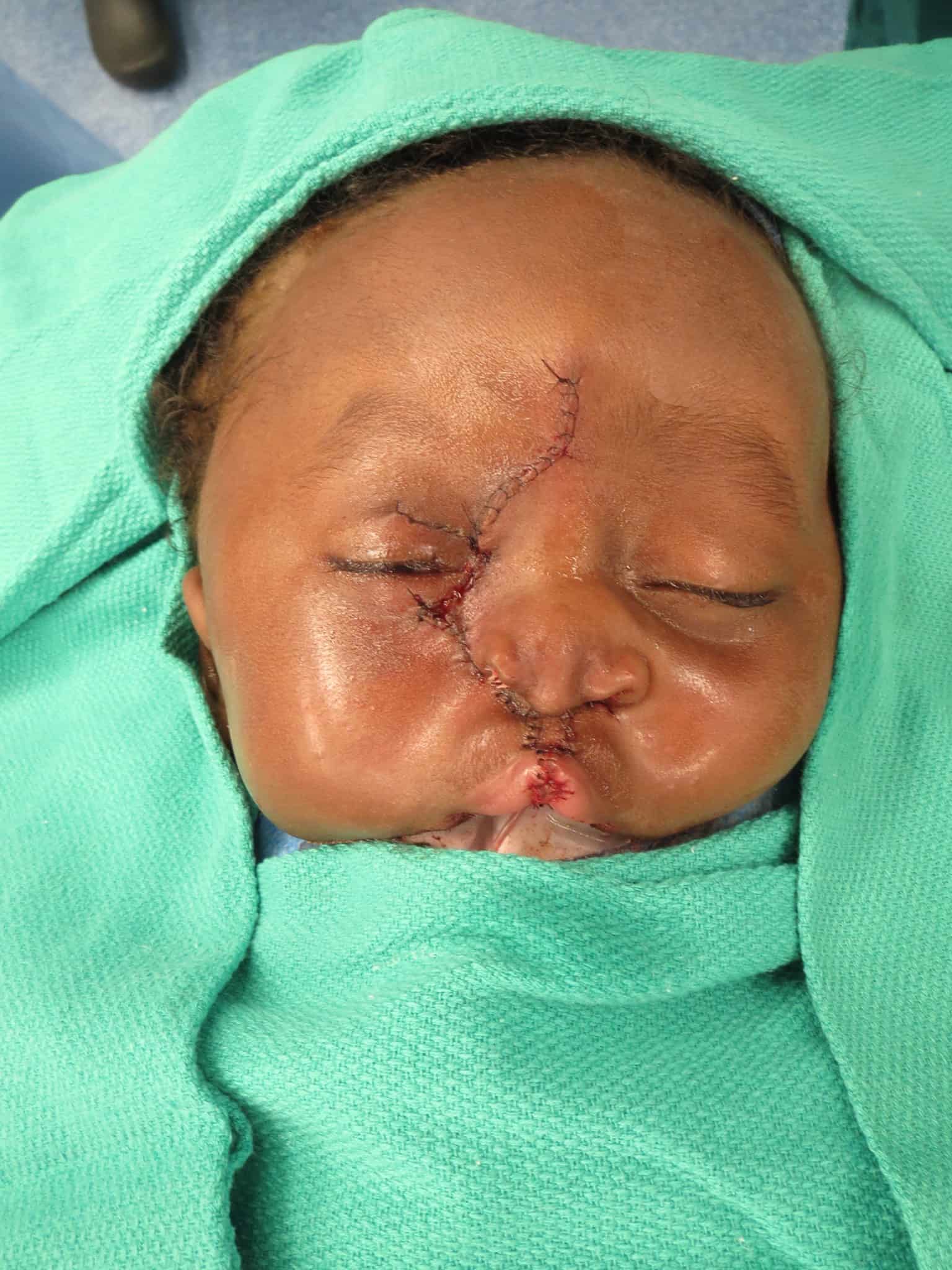
At 4 months of age, Patient 1 underwent facial cleft repair, which included all three surgeons and a combination of techniques from the three disciplines. Structures to be closed were marked on the patient’s face in advance with tattooing. The operative plan was devised in a “top-down” approach, which separated the surgery into three elements: nasal reconstruction/repositioning of the ala, cheek and eyelid repair, and bilateral cleft lip repair.
In brief, surgical techniques included the dorsal-nasal, or Reiger, flap for leveling the nasal ala, the Tenzel semicircular flap for mobilizing the medial aspect of the lower lid, the Mitek anchor for medial canthopexy, cheek advancement flaps, and a more typical bilateral cleft lip repair using fork flaps as described by Millard to provide additional tissue to create a nasal sill, as well as other advantages.
(Click on each picture for details)
Patient 2
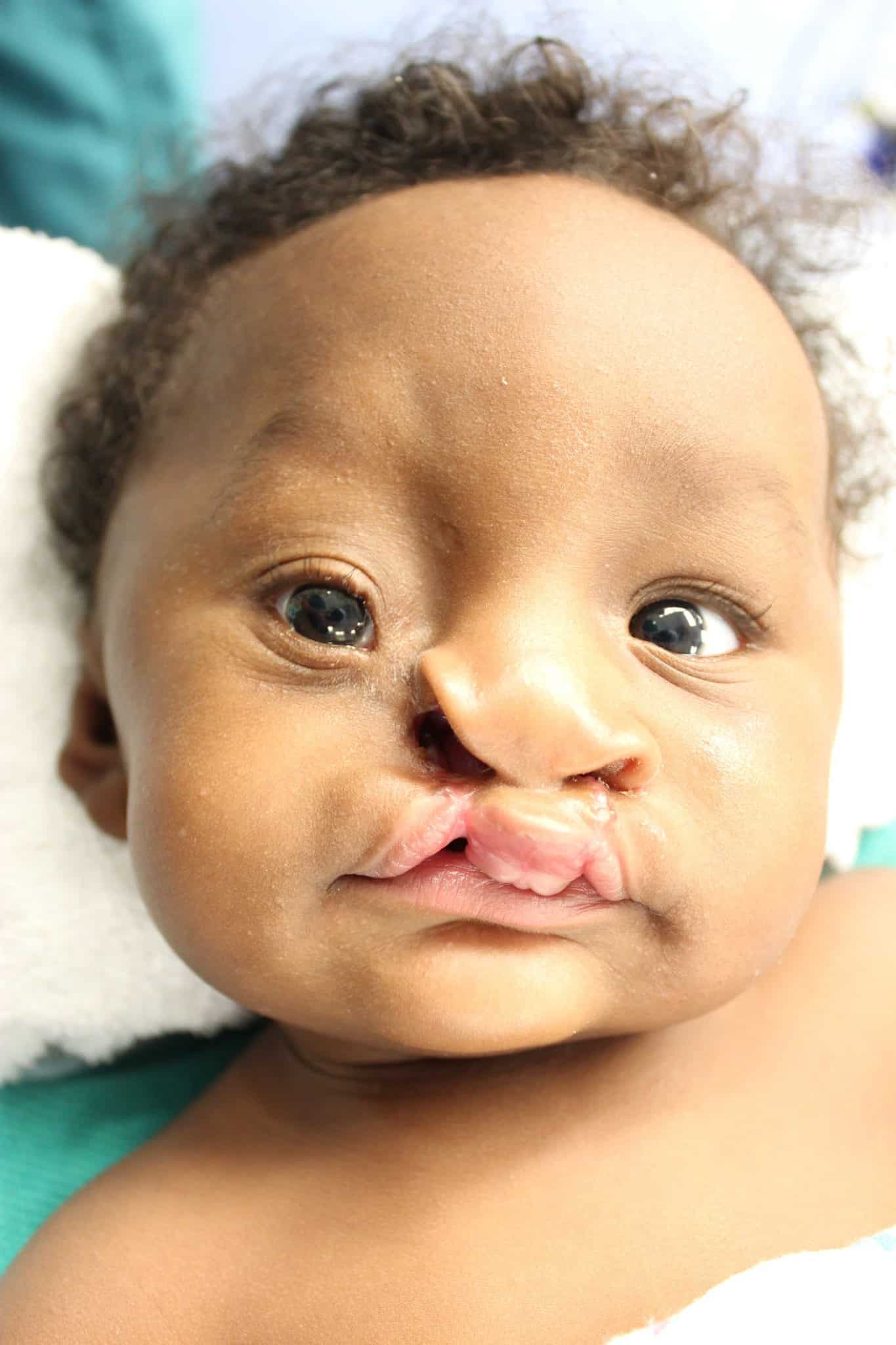
Patient 2 was remarkably similar, although her cleft was less severe and on the right side of the face. She also had a massive hydrocephalus identified prior to birth and was delivered via planned C-section at 38 weeks. She also underwent neurological procedures before undergoing craniofacial repairs.
At 1 month of age, she underwent a lip adhesion by the Seibert technique. Of note, unrelated to the Tessier cleft, VP shunt-induced craniosynostosis developed in this patient, which ultimately necessitated total cranial vault remodeling with fronto-orbito advancement.
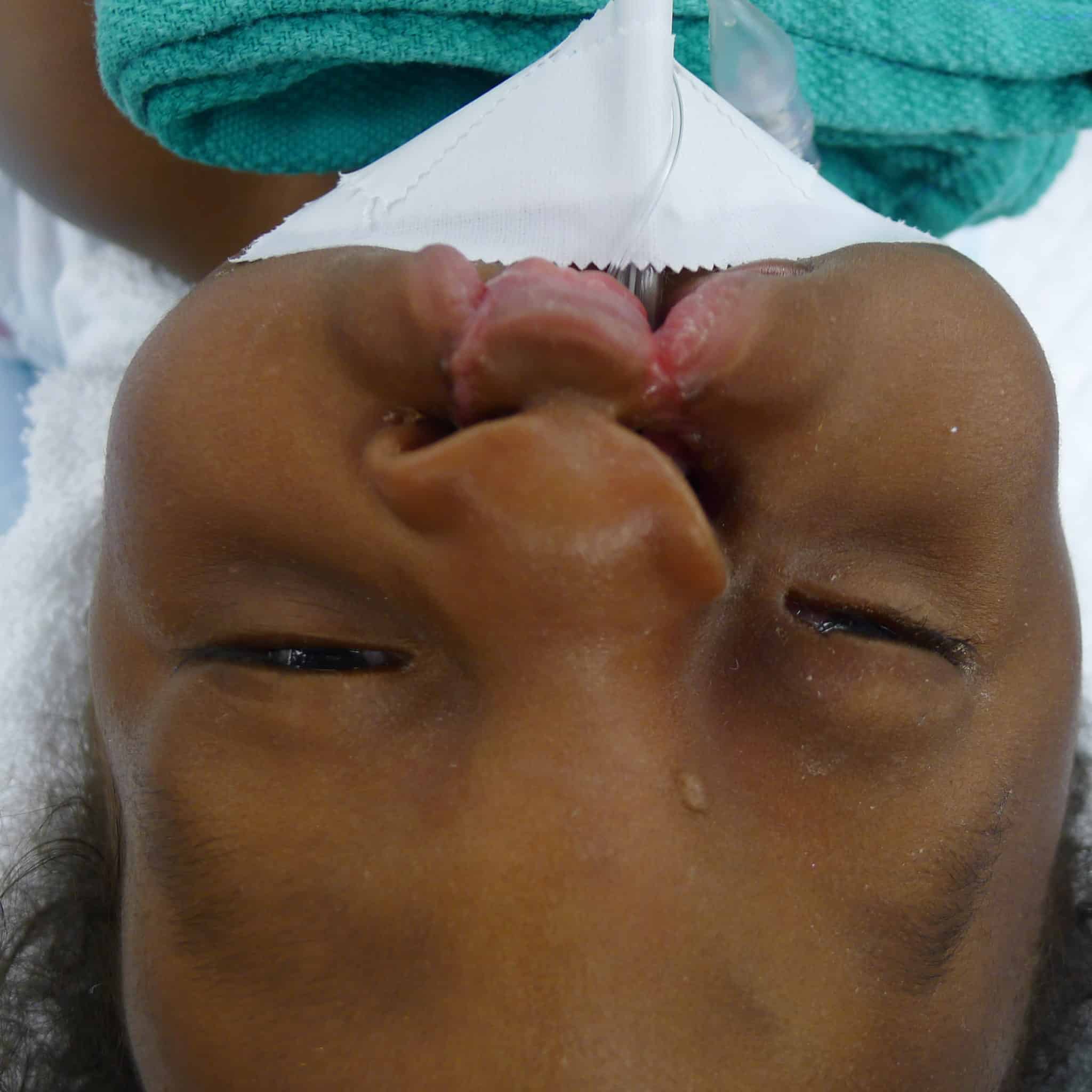
Upon oculoplastic examination, the team noted that Patient 2’s eyelid was lowered and rotated down. Unlike Patient 1, there was an island of soft tissue between the oral and ocular portions of the cleft. She had thick boney features in the prolabium that proved resistant to taping, necessitating an initial lip adhesion surgery.
Similar to Patient 1, a “top-down” approach was elected with design of a left sided, superolaterally based Reiger dorsal nasal flap with a modest back-cut.
The bilateral lip repair was performed similarly to Patient 1, with the exception of the already performed lip adhesion and still very protrusive premaxilla, which necessitated a vomer setback to better align the premaxillary segment with the lateral segments and reduce tension on the lip repair. This lip adhesion tissue was released from the lateral lip flaps and prolabial tissue and later joined together to line the premaxilla creating a separation from the lip mucosa.
The early postoperative course for Patient 2 was complicated by a minor wound infection at the glabella region managed with local wound care in addition to mild hypertrophic scarring.
(Click on each picture for details)
Follow-Ups
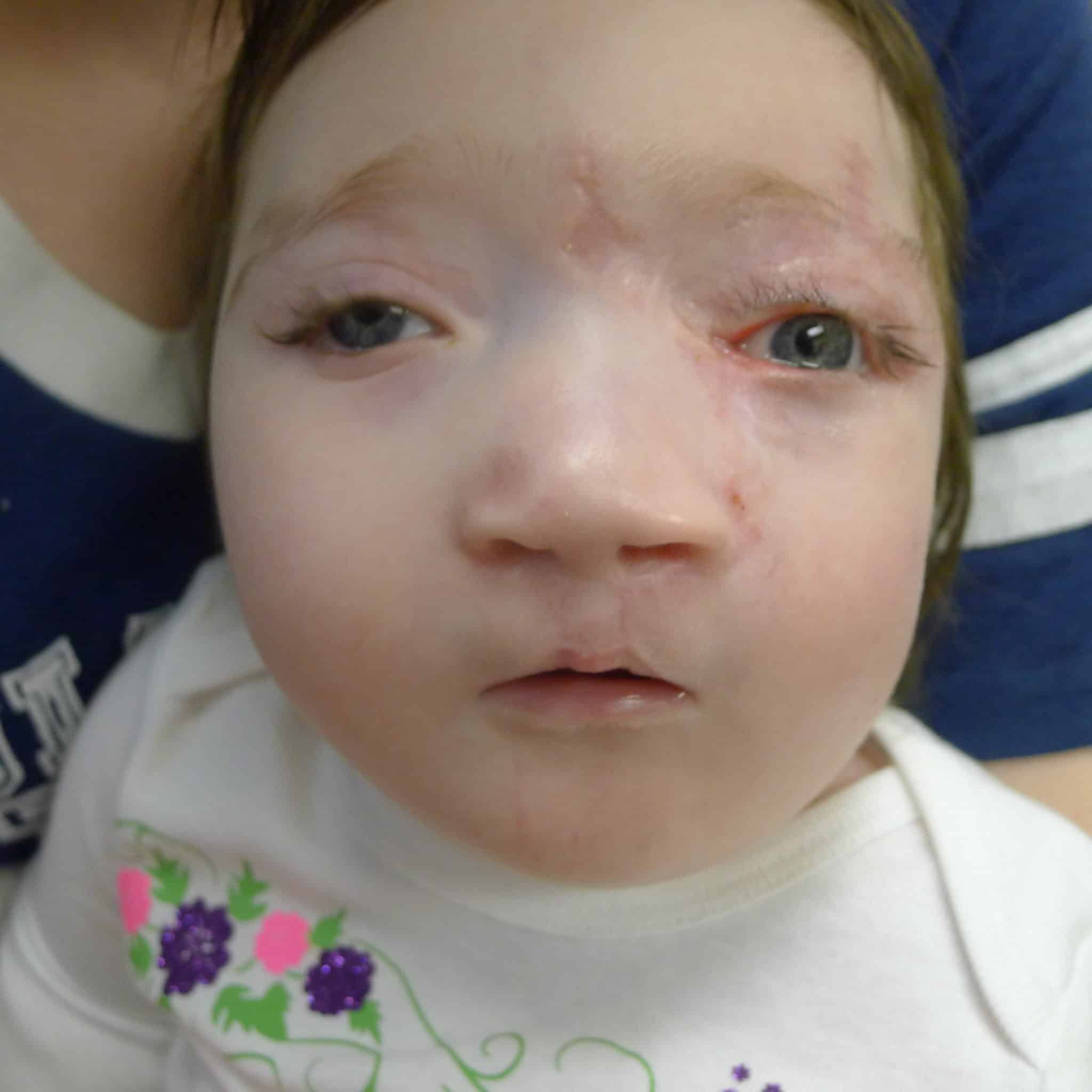
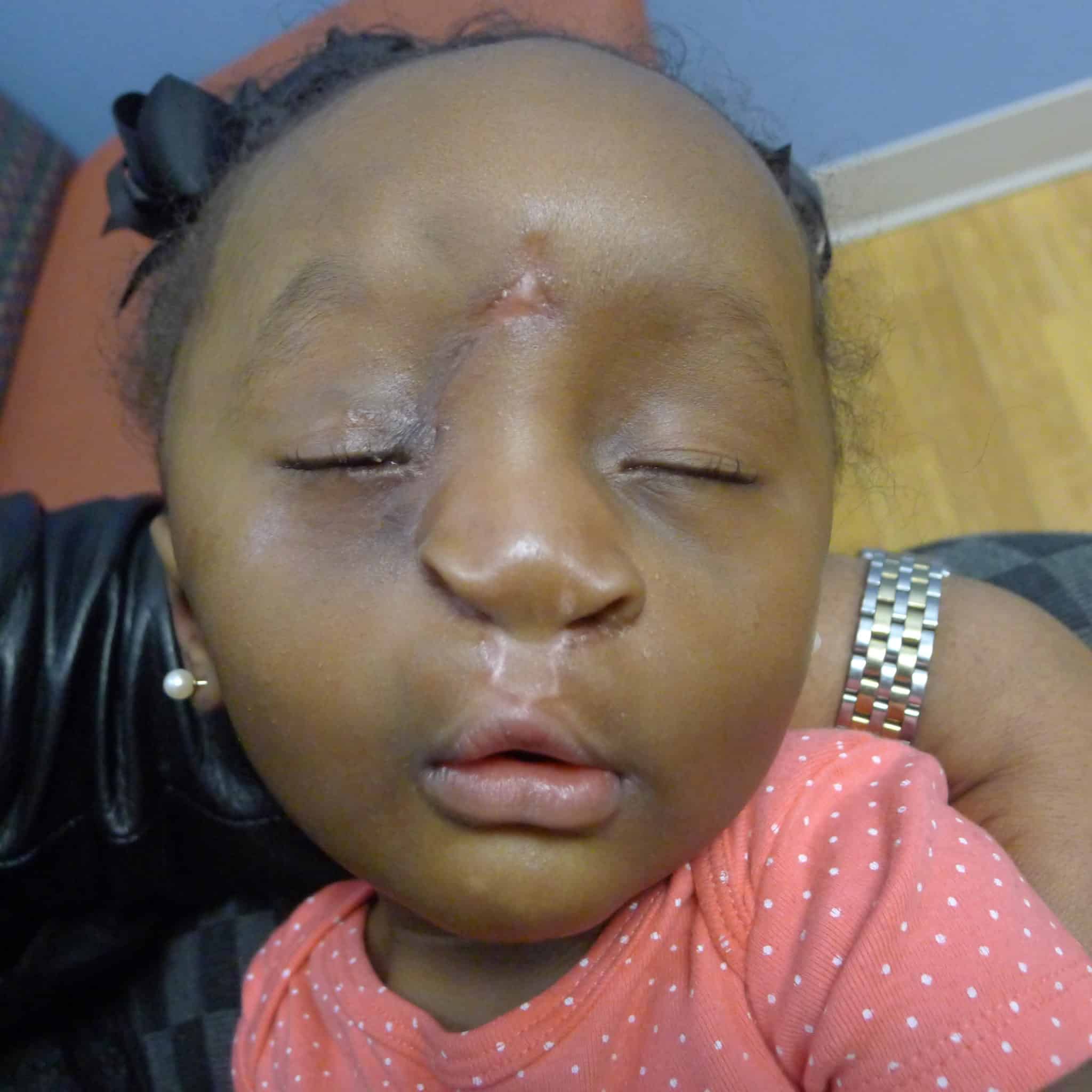
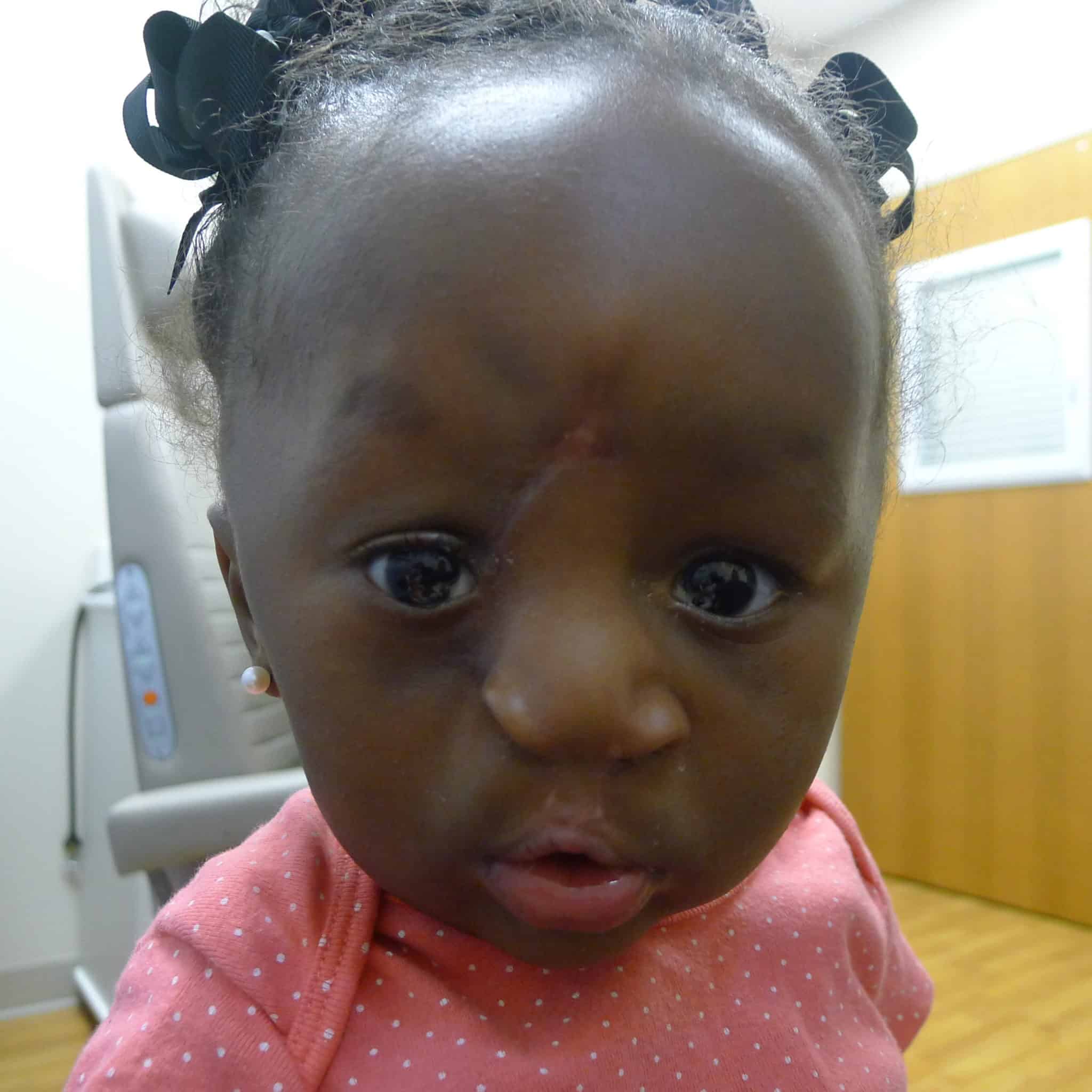
Both patients required subsequent palate surgeries and may require subsequent plastics surgeries to touch up aspects of the initial repair.
Discussion
Hartzell said these rare cases resulted in a unique opportunity to individualize care for these patients.
“I had never seen or treated a Tessier 3 during my training process, so when I began treating these patients, I was reaching out to mentors and consulting with my team at UAMS to find the best course of action,” Hartzell said. “I had to use principles that I learned in my training and in my practice and apply those in multiple ways – plus the collaborative effort of working with other specialties. In the end, we pooled skills and knowledge in a way that I truly believe gave the best outcome for these patients.”
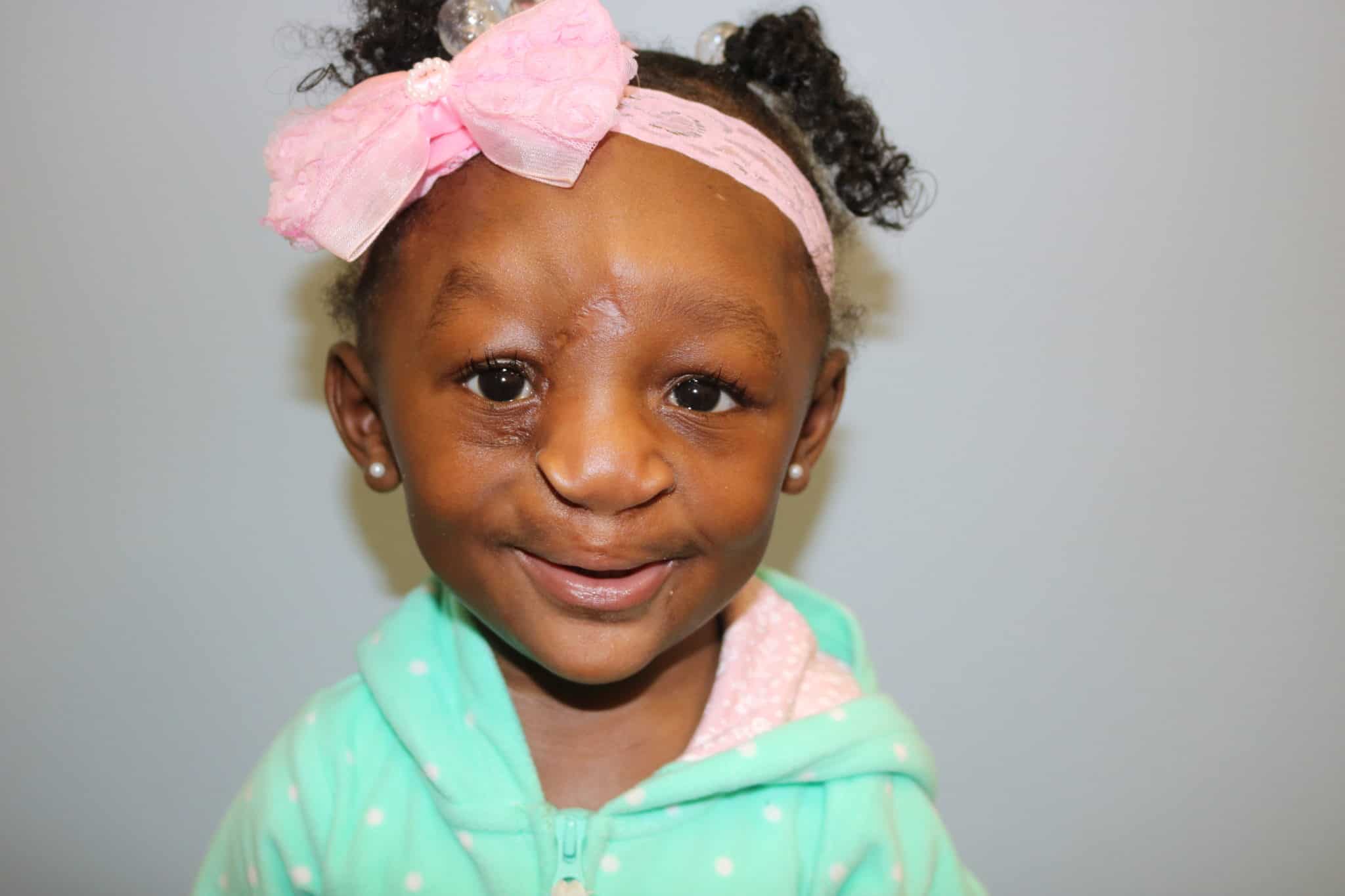
Both continue to receive care at Arkansas Children’s.
“Both girls, especially Patient 1, had poor initial prognosis and might not have survived,” Hartzell said. “They have actually surprised us all and continue to do really well. As they continue to get their care here, we continue to learn from them. And as rare as these cases are, I have since treated another patient – so the contributions of these patients and the lessons learned from this collaborative effort continue to have an impact.”
A more detailed report was published in the Journal of Craniofacial Surgery in October 2018.