By Spencer Watson
Nov. 28, 2018 | To most people, ultrasound is associated with taking pictures of babies in the womb. But it has become part of a technology revolution that is helping physicians provide better care for all types of patients.

More than 100 students from the UAMS College of Medicine as well as other medical schools in Arkansas recently gathered on the 10th floor of the Winthrop P. Rockefeller Cancer Institute for a Saturday of learning about the clinical applications of ultrasound technology.
The event, called Ultrafest, was intended to give students exposure to and hands-on experience with a variety of point-of-care ultrasound applications, from obstetrics to applications in cardiovascular and ophthalmic exams to ultrasound-guided procedures. Ultrafest was first started at the University of California Irvine in 2012. The idea for the event has since spread to several medical schools across the country. This was the first event of its kind in the Arkansas region.
“Bedside ultrasound, or what we call point-of-care ultrasound, has completely changed the way physicians care for patients,” said Brian Russ, D.O., a UAMS emergency medicine resident who helped organize the event. “As ultrasound technology gets more portable with machines becoming smaller, cheaper and better, it’s become a go-to method to make diagnoses more rapid and more accurately guide procedures at the bedside so that physicians can make better decisions and perform safer procedures in caring for patients.”
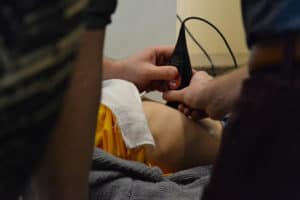
“It’s kind of a theory that bedside or even ‘pocket’ ultrasound is going to replace the stethoscope as the staple tool of the physician,” agreed John Martindale, a third-year medical student who helped organize the event.
Following a keynote address from Creagh Boulger, M.D., emergency medicine faculty and associate director of ultrasound at Ohio State University, the morning was spent with medical students learning from instructors, who demonstrated ultrasound techniques and applications on volunteer “patients,” models who were recruited from nearby universities. During lunch, students had the opportunity to form teams and compete in a fun and friendly ultrasound competition, further testing their skills and reinforcing concepts.
“We had 20 college student volunteers, most of them pre-med, who were themselves hoping to get some experience and learn some interesting things about ultrasound,” said Russ. “It was really neat for them. I was teaching the pulmonary station, and the student who was my model at the station was pointing out structures and lung artifacts, helping to teach by the end of the day.”

Of course, the volunteer patients weren’t the only ones there to learn. Medical students who attended also befitted tremendously, said Martindale, who is part of the UAMS Ultrasound Student Interest Group leadership team. Organizing the event was a significant undertaking by the student group and faculty mentors involving needs such as room and audiovisual reservations, recruiting faculty instructors and volunteer patients, advertising to students, catering and inviting industry vendors of ultrasound equipment to have enough machines for the event. Students had the opportunity to use some of the “latest and greatest” machines marketed towards point-of-care ultrasound users.
“This is technology we’ve had for decades, but the computing capacity is what’s changed. And just like any other field with computers, what we can do with that technology now is continuing to change very quickly. It’s important to stay on top of it,” Martindale said. “As a medical student, getting exposure early on, just like with anything else, makes you more proficient down the line, so when you get into residency and you’re seeing a hundred patients a day, that’s one less thing you have to learn.”
Perhaps surprisingly, many medical students don’t get consistent exposure to ultrasound during their medical education, even with its growing importance in patient care, Russ said.

“Right now, only about 25 percent of the medical schools in the United States have an integrated ultrasound curriculum, and those that do vary in degree in which the ultrasound is integrated,” he said. “We’re lucky here at UAMS. The students do get a fully integrated ultrasound curriculum during their first and second years. But what we’re doing through Ultrafest is building on their ultrasound foundation and teaching them the clinical applications and how they can make a difference for patients, with the focus on hands-on scanning time.”
Both Martindale and Russ said, with this year’s success, they plan to make Ultrafest into an annual event.
“Bedside ultrasound is quickly becoming a depended-upon resource in the medical field. Everyone is familiar with traditional uses of ultrasound in medicine — looking at babies in the womb, but the way we use it at the bedside is what has made it such as powerful tool,” Martindale said.
“We’re empowering these medical students to be the leaders in this point-of-care ultrasound revolution and to continue the change in medicine that started about 20 years ago and has continued to accelerate because of the improving technology available,” Russ said. “It’s been described as a disruptive technology in medicine because it really is changing how we provide patient care.”

















