Message from the Chairman
From the initial outbreak of COVID-19 in Arkansas to now, UAMS has been instrumental in developing a response to the coronavirus, its variants, and the inevitable impact on the healthcare system of the state and the wellbeing of the general public. And while UAMS as a whole has been the leading light, the Department of Internal Medicine has been integral to the success of day-to-day operations at the hospital, with faculty and staff tirelessly contributing to the efforts of our institution.
From early volunteers to caring for patients in the intensive care unit, Internal Medicine has set an example for professionalism and steadfast adherence to our medical mission as physicians and healthcare professionals.
While the Delta variant persists and the pandemic is far from over, it’s beneficial to look back on what we’ve accomplished so far and recognize the individuals who championed our work here at UAMS and are the HEROES of this story.

Screening
Identifying the presence of the coronavirus is imperative as we attempt to limit its spread through the community.
Thankfully, the systems we’ve put in place have resulted in effective routines at the hospital.
Giving our patient populations near and far accessible medical resources has been important, along with a focus on educating our communities on COVID-19 and best practices to remain healthy and mindful.
Drive-through screenings, mobile clinics, and community education have been foundational elements in this approach. Dr. Bob Hopkins and Dr. Michelle Krause, who have featured heavily in UAMS-led media outreach, are prominent leaders in these efforts.
Drive-through screenings have been an essential part of our early efforts to identify patients who are suffering from COVID-19 infection. The accessibility of the drive-through locations is valuable for our patients, but it also serves to reduce strain on the hospital. Dr. Hopkins has noted that “it fulfills the patients’ needs with regards to quick and effective screening, but it leaves UAMS nimble and flexible enough to meet other demands during the crisis.”
Mobile clinics demonstrate the impact of UAMS efforts to accommodate patient needs outside Little Rock. These clinics, in Central Arkansas and further out near our regional programs, have provided screening, testing, vaccinations, and education in much-needed areas. “It’s a daily challenge, but the dedication of our workers has enabled us to achieve better outcomes against COVID-19 while reaching patients that we normally wouldn’t have been able to,” said Dr. Hopkins.

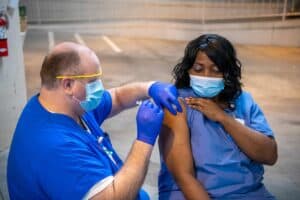
Vaccination
Preventing COVID-19 is the next big step to mitigate the number of patients hospitalized or seriously compromised by the virus. Vaccine education has been all about building relationships. The value of connecting with patients cannot be understated when discussing vaccination. Dr. Krause stresses that “understanding vaccine hesitancy in patients is paramount when working to convey the positive impact of vaccination and how it can benefit those with underlying health conditions.”
And “the ready availability of the vaccine is also useful when conferring with patients at the hospital, neighborhood clinics, or mobile sites.”
Provider vaccination was also one crucial step for creating a safe and effective work environment at UAMS when caring for COVID-positive patients. “When providers and hospital staff are inoculated against COVID-19,” Dr. Aaron Wenger says, “it builds another layer of protection and security.”
Dr. Krause also highlights the monoclonal antibody therapy that is now available for high-risk patients. The infusions of these antibodies will help to lessen the viral load and severity of illness. “It will help patients be safe to stay at home,” Dr. Krause mentions, “and they can potentially avoid hospitalization and unnecessary exposure.”
Regional programs and mobile clinics have also enabled UAMS to reach underrepresented minority populations and rural patients with effective screening, vaccinations, and the same medical access in areas that would normally be disadvantaged. These existing networks “have allowed us to provide resources for communities in need during this health crisis.”

Prevention
Understanding how infectious diseases operate is important not only for treatment of COVID-19 among the patients at UAMS but for the institution of correct protocols and safety standards at the hospital. Dr. Keyur Vyas and the Division of Infectious Disease have been implementing policies to make sure everything surrounding the treatment of COVID-19 is appropriately handled with regards to the safety of UAMS employees and the prevention of viral spread at the hospital.
The distribution and use of PPE. The process of specimens being transferred to the labs. All of the new protocols affecting patient care. Research activities where researchers are working on viruses. All of it falls under the purview of infection prevention.
In addition to all of the in-house efforts led by the Division of Infectious Disease, these physicians were also assisting the health department when the state body was buckling under the strain of the initial waves of COVID-19 infections. Dr. Vyas recalled that “we were calling every individual who tested positive, offering advice, asking how they were feeling, and answering all of the questions they might have to settle their anxiety and uncertainty. How to properly quarantine. How to stay safe. Making sure we addressed their fears.” And then all of “the pertinent information was relayed to the health department.”
Dr. Vyas concluded by noting the value of the department’s contributions during the pandemic. “We have personnel as up-to-date and informed [about COVID-19 and its treatment] as anywhere in the world. Teammates have continuously put in the time and effort over the last eighteen months and addressed challenges whenever they’ve come up. It’s been a gratifying experience to work with these colleagues.”

Patient Care
It’s inevitable, though, that patients with COVID-19 will be admitted, and, unfortunately, the volume has been incomparable to anything else we’ve encountered in the past. The contagious nature of the virus has intensified the challenges facing healthcare personnel. But through the adversity, best practices have been established, standard operation protocol has been adjusted, and healthcare professionals rallied to support one another and confront the issues that COVID-19 has presented.
Initially, care for COVID-19 patients was isolated from much of the hospital and the routines around it was not the norm for the Internal Medicine routine of care. Early volunteer efforts by physicians like Dr. Franklin Gray were pivotal in setting the tone for COVID-19 patient care and the expertise that those early volunteers developed has been valuable in transitioning patient care for COVID-19 patients from a disparate part of our non-critical care to another facet in the standard operation protocol that exists.
Dr. Wenger additionally praises physicians like Dr. Ramakrishna Thotakura and Dr. Sreelakshmi Ravula who have been intentional about researching more about COVID-19 and educating themselves and their peers. He says that inclination “to share information and maintain the basic clinical mission to meet the needs of our patients” has helped solidify the Internal Medicine approach to the pandemic in the hospital.
At the end of the day, Wenger contributes the efficacy of the non-critical patient care to the professional support that the physician and staff have extended to each other. This is the most catastrophic health care crisis in the last century, but UAMS has proven that it’s capable of confronting the pandemic and meeting the medical needs of the patients. Wenger states, “COVID is new to us, but the challenge and the adversity that the pandemic represents makes what we do as medical professionals so important and it ultimately reflects why so many of us went into medicine—to make a positive difference in the lives of people who need it.”

Critical Care
While our physicians, nurses, and medical staff endeavor to limit hospital time and speed up recovery, the severity of an illness like COVID-19 means that some patients will require critical care. Dr. Nikhil Meena and Dr. Larry Johnson have been two of our faculty members essential to the effective operation of the MICU and intensive patient care here at UAMS.
And with an increase in hospital admissions, we’ve adapted to meet the growing need.
With 18 months of the pandemic in our rearview mirror, there have been significant changes in the response to COVID-19 in the MICU. Through effective therapeutic and retrospective trials, our knowledge of the virus is better, our strategies to prevent the spread inside the hospital has improved with revised protocols, and our exposure rates our down. All of this has helped lead to reduced mortality and morbidity since last summer.
Dr. Meena also commends the nursing staff, “who have gone above and beyond to deal with COVID-19, working overtime shifts.” He also notes that “Environmental Services has helped make our spaces at UAMS safe for everyone” and “the ancillary staff who aren’t always recognized have operated as the backbone of the hospital during the pandemic.”

Research
With the potential for more variants in the future and with a long road ahead of us, it’s imperative that we discover solutions for better health care and more effective prevention and vaccination. And research is key in taking those steps. Many doctors at UAMS are working to learn more about COVID-19 and some of the trials and studies led by Internal Medicine doctors are directly responsible for greater insight into the coronavirus and treatments against it.
In her research studies, Dr. McElfish has made significant strides in address the COVID-19 disparities that Marshallese Pacific Islanders and the Hispanic community face in Northwest Arkansas. While COVID-19 does not operate in a discriminatory fashion, the inequitable socioeconomic and cultural systems in which racial and ethnic minorities live has created a disproportional burden on these minorities during the COVID-19 pandemic. And if the healthcare system forgets to acknowledge the context of how healthcare-seeking or system-avoidance behaviors emerge, then any efforts to improve vaccination behavior will be limited. Through the landmark studies with the Marshallese population in Northwest Arkansas and other ethnic and racial minorities. Dr. McElfish and her research partners have coined the term “hesitant adopter”, used to describe patients who demonstrate signs of vaccine hesitancy but who ultimately receive the vaccine despite initial reluctance. This is the only research of its kind at the moment and signals the important of community outreach and research in overcoming vaccine hesitancy.

Additionally, Dr. John Arthur collaborated with a team including Dr. Terry Harville from the Department of Pathology and numerous researchers from the Department of Microbiology and Immunology in an effort to identify the potential cause of long-lasting symptoms in COVID-19 patients.
Known as “long-haulers” these symptoms are insidious remnants of the coronavirus that patients experience after recovery. The UAMS research team has published their findings in the journal, The Public Library of Science ONE (PLOS ONE).
The discoveries shared through the findings point to an antibody attacking the ACE2 enzyme, an essential regulatory enzyme that metabolizes a peptide for immune system activation and protection. Dr. Arthur describes the research as consistently identifying “this antibody as the instigator of long COVID, so it’s an exciting development that merits further study.”
Dr. Arthur and his collaborators represented multiple departments at the hospital and demonstrated the incredible spirit of cooperation across the hospital during the pandemic. The researchers have uncovered a potential area of study that could benefit patients who suffer from fatigue, brain fog, and shortness of breath long after their initial bout of COVID-19. “This is true team science,” Arthur said. “We put together a great group of investigators that had never worked together to produce these very exciting results.”
Dr. Meena has also been very involved in medical studies during this time, acting as principal investigator on nine intervention studies, two international registries, and two prospective observational studies, all of which required extensive coordination with bedside nursing for scheduled entrances to the rooms. The logistics of these studies was complicated by the complete reworking of the consent process due to new infections prevention protocols, so the extent of Dr. Meena’s work has been both impressive and hugely valuable during the COVID-19 pandemic. UAMS has been the only site to proceed with the citrulline study that he led and patients were recruited well within the timeframe required of the study.

Unsung HEROES
Everything that we accomplish comes down to the people involved with the work. And the Department of Internal Medicine is fortunate to have an incredible roster of physicians, nurses, administrators, and support staff who are willing to go above and beyond what is required.
COVID-19 has demanded extraordinary time and effort to combat its spread and the severity of its impact on our patient population. But everyone has contributed to the continued mission of meeting our patients’ needs.
Dr. Krause comments on “the remarkable ability of the Internal Medicine department to work cohesively under stressful situations, maintaining a high-functioning level of commitment across faculty, clinical staff, and non-clinical staff.” She believes that UAMS “is a remarkable place to work during these times.
Dr. Hopkins stressed that the work at the screening and testing programs wouldn’t have been possible without the “nurses, medical assistants, APRNs, physicians, and other team members who performed a frequently thankless job, often into their off-hours.”
Codas
While the pandemic persists, the last eighteen months have demonstrated the remarkable resilience and steadfast dedication within the Department of Internal Medicine. We’ve experienced difficult days in the past and will continue to confront them in the future.
But the teamwork we display on a daily basis and the commitment to our medical mission that is maintained will always help to overcome those challenges.
Thankfully, we’re not in this alone and the contributions of everyone in our department and UAMS at large have not gone unnoticed.
To end our feature on Internal Medicine’s COVID-19 efforts, past and ongoing, we’d like to share with you some encouraging sentiments from some of the leaders in the department.
Hopkins: “When we set aside our concerns as individuals and make sacrifices for each other, we’re going to get through this, but it will take all of us pulling together. The more we do these things the less pain for everyone.”
Krause: “Thank you for all of your hard work. Day in and day out, I’ve appreciated how collegial everyone has been during these extraordinary times.”
Vyas: “There is nothing we can’t do if we put our minds to it. We’ll make it through this as long as we remember to do the best we can for our patients, trainees, and our state.”
Wenger: “We need to be asking if there is more we can do to reach out and make a stronger connection with the community around us. As physicians, we must be vigilant to not let our relationships with our patients erode so that we can fight against this together.”
Meena: “People should stop looking for the pandemic to end, but instead enjoy life as it comes and treasure what there is. Be in fellowship with the people around you, and take care of yourself and your loved ones. We’ve got to hold each other up to keep going.
While this coverage greatly exceeded the scope of a simple newsletter, many of the HEROES and their contributions were not included here. However, we do want to say “thank you” over and over again to those unsung HEROES. We shall overcome!